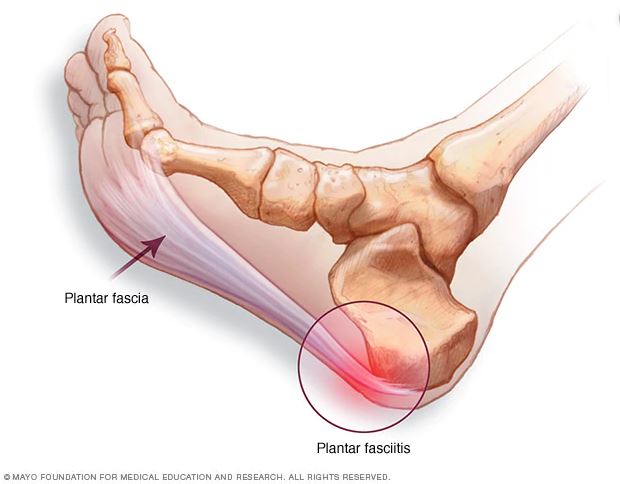
Plantar fasciitis is a condition that causes heel pain. The plantar fascia is a thick band of tissue that connects your heel to the ball of your foot. The main job of the plantar fascia is to support the arch of your foot.
What causes plantar fasciitis?
Plantar fasciitis occurs when your plantar fascia becomes inflamed (this sometimes leads to it tearing). The condition develops when repeated weight-bearing activities put a strain on the plantar fascia. People who are diagnosed with plantar fasciitis may also have heel spurs. Heel spurs are bony growths that form on the heel bone. However, people with heel spurs may not experience pain.
Plantar fasciitis affects people of all ages, both athletes and non-athletes. Men and women have an equal chance of developing the condition.
Factors that contribute to the development of plantar fasciitis include:
- Age (over 40 years)
- A job, sport, or hobby that involves prolonged standing or other weight-bearing activity
- Rapid increases in length or levels of activity, such as beginning a new running program or changing to a job that requires a lot more standing or walking than you are accustomed to
- Decreased calf muscle flexibility
- Increased body weight (Body Mass Index greater than 30)
- Tendency to have a flat foot (pronation)
How do I know if I have plantar fasciitis?
If you experience pain when you put weight on your foot—particularly when taking your first steps in the morning, then you may have plantar fasciitis. The pain can be felt in your heel, or along the arch and the ball of your foot.
The onset of symptoms of plantar fasciitis frequently occurs with a sudden increase in activity. You might feel a stabbing pain on the underside of your heel and a sensation of tightness and/or tenderness along your arch.
People with plantar fasciitis may experience pain:
- In the morning, when stepping out of bed and taking the first steps of the day
- With prolonged standing
- When standing up after sitting for awhile
- After an intense weight-bearing activity such as running
- When climbing stairs
- When walking barefoot or in shoes with poor support
As your body warms up, your pain may actually decrease during the day, but then worsen again toward the end of the day because of extended walking. Severe symptoms may cause you to limp.
How is plantar fasciitis diagnosed?
Our physical therapist’s diagnosis is based on your health and activity history along with a clinical evaluation. Additionally, your therapist will ask about your medical history to make sure that you don’t have other possible conditions that may be causing the pain.
Sharing information about the relationship of your symptoms to your work and recreation, and reporting any lifestyle changes, will help your physical therapist diagnose your condition. Your physical therapist will then tailor a treatment program for your specific needs.
How does a physical therapist treat plantar fasciitis?
Our highly trained physical therapists are more than capable of treating plantar fasciitis. As a matter of fact, we treat many patients here at Impact Rehab & Wellness for plantar fasciitis.
Our physical therapists use the following techniques to treat plantar fasciitis:
- Fascia Mobilization: Mobilization of the fascial adhesions on the plantar surface of the foot is essential to improve pliability for weight bearing demands. While ball rolling on the bottom of your foot to address muscle tension can assist with mobility, it usually is not deep enough to localize restrictions. Not only can our physical therapists more specifically target primary restricted regions, but they can also address limitations in ankle and foot mobility. These limitations can prohibit your foot from adapting to the ground for even weight distribution with walking.
- IASTM: Instrument Assisted Soft Tissue Mobilization uses uniquely crafted tools to target connective and soft tissue restrictions. Our physical and occupational therapists are trained in this technique. Using IASTM, they can directly localize restricted regions to remodel the fascial adhesions causing stiffness, limited mobility, and chronic pain. Improving mobility and pain will serve to restore function of your foot.
- Functional Dry Needling: Functional Dry Needling is a form of trigger point therapy. It’s intended to release restrictions in muscles that result in pain and altered movement. While the plantar fascia is not directly treated, addressing “knots” in your calf and hamstring muscles provides relief.
- Kinesiotaping: Kinesiotaping is a rehabilitative taping technique that promotes the natural healing process of your body. It does this by providing support to your muscles. This helps improve function without limiting natural mobility. Patients who have an improvement with taping may also benefit from orthotics.
- Evaluation of Running/Walking Mechanics: Physical therapists are trained to recognize muscle weaknesses and imbalances. Additionally, they understand how these deficits can impair the functions of walking or running. Your physical therapist will analyze your muscle function. This will enable them to prescribe exercises that will address observed deficiencies.
- Selection and Instruction in Exercises: Our physical therapists can provide you with exercises that will target muscle tightness as well as weakness. A thorough evaluation of your hip, knee, ankle, and foot is necessary. Weakness or tightness in any of these areas could be contributing to your plantar fasciitis. Once these areas are assessed, your physical therapist will be able to provide you with proper instruction of exercises.
What now?
If you feel that you might be suffering from plantar fasciitis, give us a call! We will do a free, 15 minute assessment. If our physical therapists determine that you have plantar fasciitis, we will schedule you an appointment. Our physical therapists will work hard to get you back to feeling better!
